|
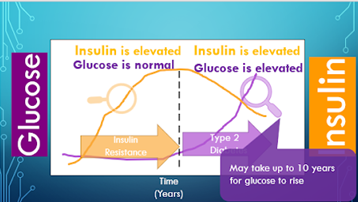
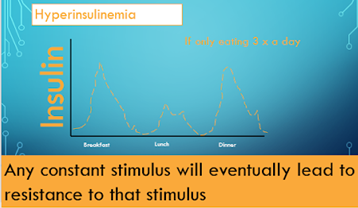
A problem with our current diagnosis of metabolic health is our obsession with monitoring glucose and viewing as the metric that matters. In the example below we have the two time points. The first is Insulin Resistance or pre diabetes and important to note the glucose is normal but insulin is elevated they are not the same thing we fail to appreciate that they do not go hand in hand that if glucose is low insulin is low or glucose is high insulin must be high. For an historical point- Dr Joseph Kraft a pathologist developed the kraft test- an Oral glucose tolerance test with insulin assessment. Testing over 15,000 patients he found that in over 50% of confirmed diabetes cases they had normal glucose levels but high insulin. This would have been missed if we only test blood glucose levels. Glucose is obsessively the marker we concentrate on with diabetes but it shouldn’t be! We have the ability to measure insulin, so why don’t we? We see here that insulin is highlighting the problem potentially 10 years before we see a change in blood glucose levels. This is the potential if we come away from a glucose centric paradigm. How is hyperinsulinemia caused? The first eating pattern of 3 meals a day is more of an uncommon eating pattern we see today. Every time you eat this is the reciprocal insulin response across the day.
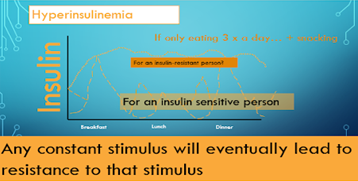
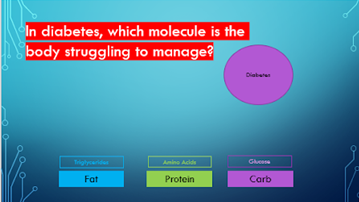
Compare that to the more common pattern of breakfast, mid morning snack, lunch, mid afternoon snack, dinner and possibly dessert. This causes many more insulin responses and with a insulin sensitive person this can be managed for a while. But for an insulin resistant person the insulin never comes down it is constantly elevated. Therefore, we can now see that hyperinsulinemia can be a consequence of insulin resistance and also a cause. Its a vicious cycle accelerating the problem until the person changes their habits. How do we correct insulin resistance? If hyperinsulinemia is the primary cause then lowering insulin needs to be the solution. We do that through the foods we eat and by managing these macro nutrients. Compared to drugs it doesn’t come along with side effects it actually has side benefits to all our metabolic markers and our waistline! How do Macro nutrients affect Insulin? Currently according to the global nutrient database this is the proportion of macro nutrients we are eating around the world, Carbohydrates were the major contributor to energy availability (70·5%), followed by fats (17·4%), and protein (10·5%). Fat does not increase insulin, there is no study that shows that according to Dr Ben Bikman PhD. Protein has a small effect but carbohydrates have a large effect (18). In the image below this is the effect size in a slightly different view. This is not declaring a war on carbs because the type of carbohydrates do matter, but when we acknowledge that hyperinsulinemia is the cause of insulin resistance, one of these diets is going to work much better at removing the offending agent. When we eat these macro nutrients there is a corresponding blood molecule. In diabetes (type 2) which is just a prolonged insulin resistance, which of these nutrients in the blood is the body struggling with. Glucose is the one we obsess over the most and the one we are all eating the most of. “If lifestyle is the culprit, it is also the cure! The food we eat is causing or can cure these metabolic issues! When we look through an insulin lens, we appreciate we just need to lower the insulin by managing our macro nutrients, control carbohydrates, prioritise protein, don’t fear fat, and maybe frequently fast. This can literally cure the problem.” Dr Ben Bikman
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Taylormade
|
PERFORMANCE AND REHABILITATION CLINIC
Injury Management and Conditioning Specialist
Taylormade Rehab, 1 Belle Vue, Fenny Bridges, Honiton, Devon EX14 3BJ | 07800 824557 | 07855 386634
© 2019 Taylormade | Performance & Rehabilitation Clinic. Injury Management & Conditioning Specialists | Website design by brightblueC
© 2019 Taylormade | Performance & Rehabilitation Clinic. Injury Management & Conditioning Specialists | Website design by brightblueC


 RSS Feed
RSS Feed
